UK HealthCare Pulmonary Rehab Clinic Helps Covid-19 Patients Get Back on Their Feet
LEXINGTON, Ky. (Sept. 11, 2020) — Rounding the curve of Alumni Drive as the grand site of Kroger Field comes into view usually fills people with excitement.
But in April, all Charity Bowlin felt was fear.
"I saw the stadium and I just started crying," she said. "I told my husband, 'I'm going to be here for a while. I know I'm really sick.'"
Bowlin's destination wasn't Kroger Field. Instead she was headed just beyond it - to UK HealthCare's Chandler Emergency Department - dangerously short of breath with a positive COVID-19 diagnosis.
Coming down with COVID
Bowlin, of Williamsburg, Kentucky, worked for a nursing home in Jackson County, which is where she believes she became infected.
She noticed her first symptom on Thursday, April 2.
"I will never forget that day as long as I live," Bowlin said. "I have allergies, so I constantly have a runny nose, but that Thursday, my nose was stuffy. That never happens unless something is wrong."
Bowlin called into her local doctor for a telehealth visit from work. She was diagnosed with a sinus infection and prescribed a round of antibiotics, but she woke up the next morning around 2 a.m. with a high fever. By the weekend, Bowlin lost her taste and smell. She drove to her family physician's office first thing the following Monday for a COVID test, which came back positive two days later.
"By then, I was coughing so bad that I couldn't catch my breath. I struggled through the whole day," Bowlin said. "I borrowed one of my mom's oxygen tanks because I could tell my sats were dropping. I told my husband - it's time to go to Lexington."
A 15-day stay
After arriving at UK Chandler Hospital, Bowlin said she was immediately hooked up to oxygen, as her oxygen sats were reading 83%.
"I was afraid that the doctors would be scared to take care of me," Bowlin said. "That could not have been further from the truth. They made me feel so comfortable. They were not afraid to come into my room and help me even though I had this terrible disease."
Bowlin had developed other symptoms including nausea, headaches and high blood pressure. She knew her health was in serious jeopardy and she wanted her doctors to be upfront about her condition. She was ultimately diagnosed with pneumonia and placed on high-flow oxygen (HFO) therapy to give her lungs a break.
*****
Thankfully, HFO therapy was the break Bowlin needed. After a few days, she started to feel better - well enough to answer messages from numerous family members and friends who reached out to check on her.
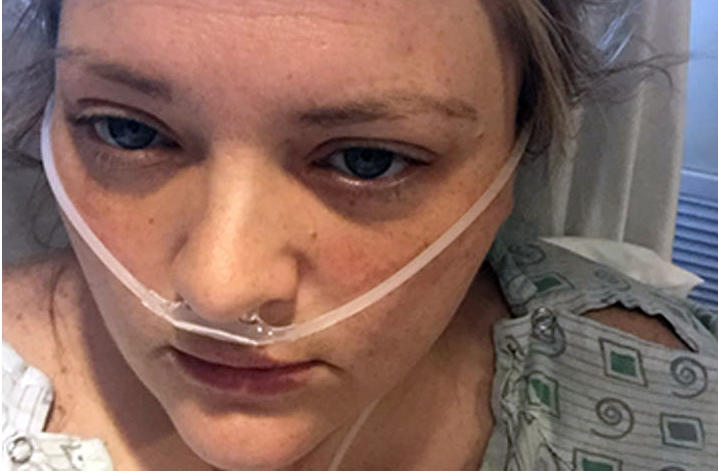
It was one of her friends who suggested Bowlin document her journey to recovery.
"I took pictures each day. I wanted to show how real this disease is," Bowlin said. "Normally, I would never post pictures of myself looking like I did, but it was my real-life, raw situation and there are so many others who have a much worse outcome than me."
While isolation was difficult, Bowlin said her nurses and doctors went above and beyond to make her feel less alone and afraid.
"They treated me like family. I thank the Lord every day for everyone who took care of me," she said.
Recovery and Beyond
Months after her COVID ordeal, Bowlin still suffers physical and mental challenges, many of which she struggles to deal with alone.
An integral part of her continued recovery includes visiting UK HealthCare's Pulmonary Rehabilitation Clinic at its new location in the Kentucky Clinic.
"We see many COVID-19 patients who are continuing to recover," Bryan Collins, supervisor of UKHC's Pulmonary Diagnostic Laboratory & Pulmonary Rehabilitation, said. "Suffering through a COVID diagnosis, especially for patients who are hospitalized, is traumatic and stressful for a person's body and can have damaging effects that last well beyond their hospital stay. Rehabilitation is imperative to help our patients heal."
Pulmonary rehabilitation is a comprehensive program that helps patients regain the ability to live normal day-to-day lives and restore independence. The pulmonary rehabilitation program at UK is based on a team approach - including pulmonologists, nurses, exercise physiologists, dietitians and therapy technicians - who work with each patient to develop an individualized treatment plan.
"Each participant is followed closely to ensure an appropriate exercise prescription, dietary plan and medication plan," Collins said. "We evaluate the patient's progress to make sure they are making improvements."
Most people who undergo pulmonary rehabilitation have chronic obstructive pulmonary disease (COPD); however, people who have chronic bronchitis, emphysema, pulmonary fibrosis, or pulmonary hypertension may also benefit from rehab.
Bowlin's rehabilitation included a 12-week outpatient program. Since she lives more than an hour away from Lexington, a majority of her visits were via telehealth. Her physical therapist, Angela Steele, said the telehealth visits are just as important as those in-person.
"We were still able to monitor her vital signs with exercise," Steele said. "A lot of our patients appreciate the virtual visits because it saves them a trip to Lexington, but still gives them access to the essential care that they need for recovery."
"I remember vividly my first visit," Bowlin said. "I was crying a lot because I was having so much trouble doing the exercises I was being asked to do, even though I normally would have no problem completing them."
Bowlin was tired. She was still experiencing anxiety and having trouble sleeping.
"I was getting two, maybe three hours of sleep a night for a week and a half," she said. "I suffer from post-traumatic stress disorder (PTSD) and often find that small things trigger me. I cried in the shower one night because I remembered how my husband had to help bathe me once I was home from the hospital because I was still so weak."
With the help of Steele and a lot of determination, Bowlin started to improve. After 12 weeks, she was able to walk on the treadmill for 30 minutes - a major accomplishment after her COVID ordeal.
"I was knocking on death's door and here I was, finally able to walk for 30 minutes without stopping," she said. "It has given me the confidence to continue recovering."
As the state’s flagship, land-grant institution, the University of Kentucky exists to advance the Commonwealth. We do that by preparing the next generation of leaders — placing students at the heart of everything we do — and transforming the lives of Kentuckians through education, research and creative work, service and health care. We pride ourselves on being a catalyst for breakthroughs and a force for healing, a place where ingenuity unfolds. It's all made possible by our people — visionaries, disruptors and pioneers — who make up 200 academic programs, a $476.5 million research and development enterprise and a world-class medical center, all on one campus.