‘UK became our home’ — DanceBlue Clinic patient, mom focus on the positives
LEXINGTON, Ky. (March 23, 2023) — “We thought it was a spider bite — we didn’t think much of it.”
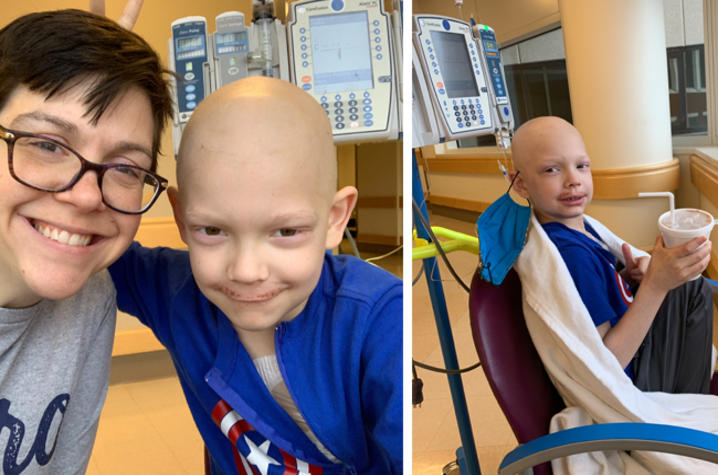
That’s what Richmond residents Dynae Utz and her husband, L.T., thought when they first saw the lump on their 6-year-old son Lewis' leg. Then the lump got bigger, to the point where surgery was needed to remove it.
Lewis’ surgery came with some complex timing. On July 9, he had the lump removed by surgeon at Kentucky Children’s Hospital. Just four days later, Dynae underwent a cesarean to deliver her son PJ. While still recovering from delivery, Lewis’ surgeons visited her in her hospital room. The lump came back from pathology, and they wanted to discuss the results with her.
“I just knew,” said Dynae. “I just knew in my gut it was cancer. You don’t come to my hospital room with good news.”
Dynae’s mother had just passed from a rare cancer the previous September. Cancer had been her whole world for months, and here it was again. Three days after giving birth, Dynae went from the labor and delivery unit to the DanceBlue Kentucky Children’s Hospital Hematology/Oncology Clinic, just one floor away, to discuss what was next for Lewis’s treatment.
“They didn’t know what type it was,” Dynae said. “They were talking ports and scans and all these things that were really hard to hear about your 6-year-old. And I just had a baby who was downstairs in the NICU. My emotions were everywhere.”
Between Lewis’ surgery, the premature birth of her son PJ and her complex delivery and surgery, Dynae and her family spent the better part of a month at the University of Kentucky Albert B. Chandler Hospital. Two days after PJ was discharged from the neonatal intensive care unit (NICU), Lewis began chemotherapy for what turned out to be a very unique cancer.
“Lewis has a type of sarcoma called CIC-DUX4 sarcoma,” said Caryn Sorge, M.D., Lewis’s oncologist. “This is a soft-tissue type of cancer and can be very aggressive.”
Unlike Ewing sarcoma, a more common tissue and bone cancer found in children and adolescents, CIC-DUX4 is a relatively new and rare cancer that can spread very quickly. Dynae and her husband were desperate to find more information, but there was little to be found. Internet searches were futile, as there are only a handful of publications and no clinical trials or studies they could enroll Lewis in. The best course to treat CIC-DUX4 is similar to how Ewing sarcoma is treated — radiation, chemotherapy and surgery.
“Ewing has a high survival rate — this one does not,” said Dynae. The cancer spread to Lewis’s lungs, and the Utzes had to go to Cincinnati Children’s Hospital for a highly specialized surgery to remove the spots. Still reeling from her mother’s death, Dynae faced Lewis’ illness the only way she knew how.
“I had to ‘just keep swimming’ and power through for Lewis,” she said. “I tried to keep a positive attitude. I don’t know how else to be but to be happy and a little bit of sunshine in a sad situation.”
Because of COVID restrictions, they couldn’t interact with other patients or families. But Dynae made it a point to take Lewis on “dates” around the hospital. They would look out the windows to UK’s Kroger Field. With the help of KCH’s Child Life staff, they had hot chocolate, movie nights and picnics.
“We tried to make it as fun as possible,” said Dynae. “There’s only so much you can do in a hospital room.”
Behind her positive outlook, Dynae was wracked with guilt.
“The mom guilt is real hard,” she said. “It was like, what did I do when I was pregnant? How did I mess this up? And I know it wasn’t my fault, but it’s one of those things you think about.”
Lewis’ last day of radiation was July 13, 2021 — almost exactly one year from his first surgery. In the chemotherapy sessions that followed, Dynae and her husband noticed a change in Lewis’ behavior.
“Before chemo, he had some sensory issues,” she said. “But then things started getting more pronounced. He would get angry. Not in normal, ‘I have cancer,’ 6-year-old way. But in a violent, impulsive way.”
Lewis was diagnosed with level 1 autism spectrum disorder. It was theorized that his cancer treatment could have potentially exacerbated Lewis’ autism, as some chemotherapy drugs can cause neurotoxicity.
“His chemotherapy can have neurotoxicity as an acute side effect,” said Sorge. “It is hard to say exactly if it made his autism worse but certainly going through all that he did can be difficult to adjust to for any child, especially a child with autism.”
“Before, he could understand social contracts,” Dynae said. “He could understand things like, ‘You don’t say things that hurt other people’s feelings.’ But now he’s much more impulsive, and we’re working on behavior and understanding social cues. But he’s still so friendly and loving.”
Through it all, Dynae found support in a network of other parents of children in the DanceBlue Clinic. During Lewis’s extended inpatient stays, COVID restrictions meant that she couldn’t lean on other parents going through a similar experience. But now that Lewis is in remission and doing well, Dynae is able to offer the kind of support that she knows other caregivers need.
“I know that feeling,” she said. “You know you didn’t screw up, but you feel that way. I’m just another mom going through the same thing. You can call me.”
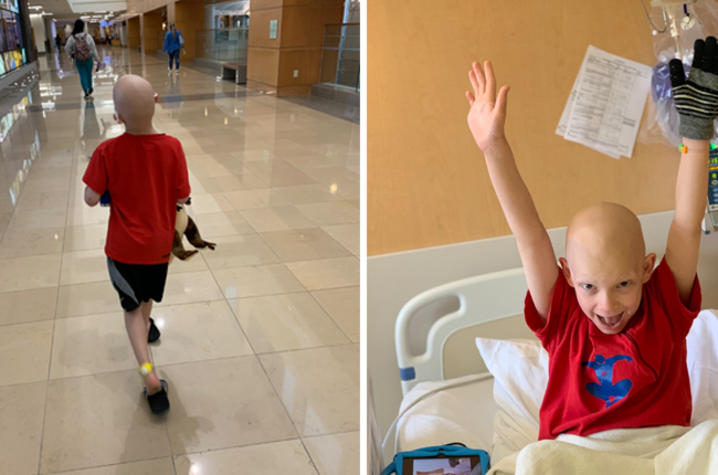
Lewis is currently in remission and doing well. Since his type of cancer does have a high rate of reoccurrence, he returns to the DanceBlue clinic for X-rays and MRIs every three months. According to Sorge, Lewis hasn’t shown any evidence of the cancer’s return.
And Lewis will tell that to anyone who will listen. Dynae describes Lewis as the ultimate advocate for himself. They talk about the tests, scans, results and what they mean. At school, he’s excited to tell his classmates all about MRIs, how they work and what it’s like to get scanned.
“It gives him a lot of confidence, that he can talk about something like that,” Dynae said. “He’s really cavalier about his cancer. He’ll talk to you all day about it.”
Aside from the periodic checkup, Lewis, now 9 years old, is back to being a kid. He goes to school, collects and trades Magic cards and loves roller coasters. He and Dynae are excited about reuniting with his care team and the student volunteers at the 24-hour DanceBlue Marathon March 25-26. And for Dynae, she’s looking forward to the opportunity to meet with other parents and caregivers and support them in any way she can.
“UK became our home — we lived there for a year,” she said. “That’s my goal in all of this. If what we went through can help anybody else, that’s what I want to do.”
UK HealthCare is the hospitals and clinics of the University of Kentucky. But it is so much more. It is more than 10,000 dedicated health care professionals committed to providing advanced subspecialty care for the most critically injured and ill patients from the Commonwealth and beyond. It also is the home of the state’s only National Cancer Institute (NCI)-designated Comprehensive Cancer Center, a Level IV Neonatal Intensive Care Unit that cares for the tiniest and sickest newborns and the region’s only Level 1 trauma center.
As an academic research institution, we are continuously pursuing the next generation of cures, treatments, protocols and policies. Our discoveries have the potential to change what’s medically possible within our lifetimes. Our educators and thought leaders are transforming the health care landscape as our six health professions colleges teach the next generation of doctors, nurses, pharmacists and other health care professionals, spreading the highest standards of care. UK HealthCare is the power of advanced medicine committed to creating a healthier Kentucky, now and for generations to come.